Snoring vs Sleep Apnoea – When Should You Be Concerned?
Snoring is often brushed off as a harmless annoyance, yet it can sometimes signal a deeper sleep-related breathing issue. As an ENT doctor, I regularly see patients who assume their snoring is normal, only to discover an underlying airway problem that requires proper medical attention. Understanding the difference between simple snoring and sleep apnoea is essential because one is mainly disruptive, while the other can affect long-term health.
This article explains how snoring and sleep apnoea differ, why the distinction matters medically, and when it is sensible to consult an ENT specialist. The goal is to help you recognise warning signs early and make informed decisions about assessment and treatment.
Snoring vs obstructive sleep apnoea: what’s actually different?
What is snoring in clinical terms
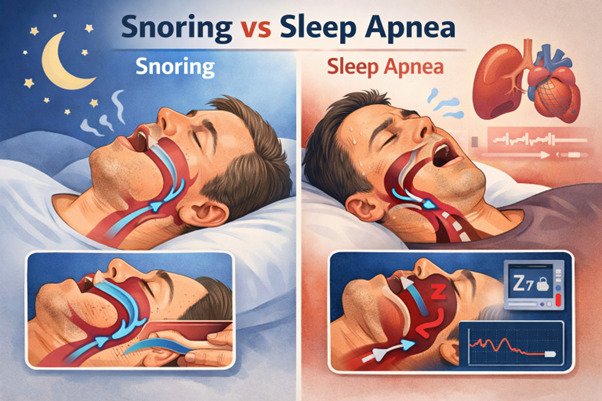
Snoring occurs when airflow through the upper airway becomes partially restricted during sleep. As air passes through narrowed spaces, soft tissues such as the soft palate and throat vibrate, producing sound. In many people, snoring is intermittent and does not significantly disturb breathing or oxygen levels.
What obstructive sleep apnoea really means
Obstructive sleep apnoea is a sleep disorder in which the upper airway repeatedly narrows or collapses during sleep. These episodes cause breathing pauses, drops in oxygen levels, and frequent brief awakenings that fragment sleep. Unlike simple snoring, sleep apnoea places strain on multiple body systems over time.
Why the distinction matters medically
The key difference is not the volume of snoring but its effect on breathing and sleep quality. Snoring alone may be socially disruptive, but sleep apnoea is linked with excessive daytime sleepiness and reduced cognitive performance. When left untreated, it may contribute to more serious health concerns.
Warning signs that snoring may be more than “just snoring.”

Night-time symptoms to watch for
Loud, habitual snoring that occurs most nights can be an early warning sign. Breathing pauses, choking, or gasping sounds during sleep are particularly concerning. Some individuals also wake with a dry mouth, sore throat, or morning headaches.
Daytime symptoms that raise concern
Persistent tiredness despite adequate time in bed is a common red flag. Many patients report difficulty concentrating, memory lapses, irritability, or reduced productivity. These symptoms suggest poor-quality sleep rather than insufficient sleep duration.
Situations where risk is higher
Snoring that worsens with weight gain or alcohol intake deserves closer attention. Symptoms that progress with age or occur alongside other medical conditions should not be ignored. In such cases, an ENT assessment can help determine whether sleep apnoea is present.
What causes snoring and sleep apnoea from an ENT perspective
Where airway obstruction usually occurs
From an ENT viewpoint, both snoring and sleep apnoea result from narrowing in the upper airway. This may involve the nose, soft palate, tonsillar region, tongue base, or several levels at once. Sleep apnoea often reflects more extensive airway collapse than simple snoring.
Common nasal contributors
Chronic nasal blockage can significantly worsen snoring and sleep-related breathing disorders. Causes include allergies, sinus inflammation, enlarged turbinates, or a deviated nasal septum. Poor nasal airflow encourages mouth breathing, which increases airway instability during sleep.
Throat and soft tissue factors
Enlarged tonsils, a long soft palate, or a bulky tongue can narrow the space behind the mouth. During sleep, natural muscle relaxation allows these tissues to fall back more easily. This effect is particularly pronounced in sleep apnoea.
Lifestyle and physiological influences
Alcohol and sedative medications relax airway muscles and can worsen airway collapse. Excess body weight may add soft tissue around the neck, reducing airway diameter. These factors are important considerations during ENT assessment and treatment planning.
What an ENT assessment usually involves
A detailed clinical history
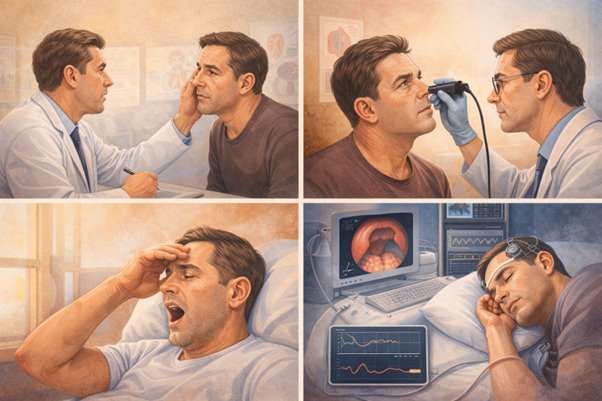
An ENT consultation begins with a careful review of symptoms. This includes snoring patterns, witnessed breathing pauses, sleep quality, and daytime alertness. Information from a bed partner often provides valuable insights.
Examination of the upper airway
The nose, mouth, throat, and neck are examined in detail. In many cases, a flexible endoscope is used to visualise internal airway structures. This allows precise identification of anatomical contributors to obstruction.
Sleep studies and diagnostic testing
If sleep apnoea is suspected, a sleep study is usually recommended. This test measures breathing patterns, oxygen levels, and sleep stages overnight. The results confirm the diagnosis and help determine severity.
Additional tests when required
Further investigations may be considered in selected cases. These are typically used when anatomy is complex or when procedural treatment is being evaluated. Testing is tailored to individual clinical needs.
Treatment approaches: how snoring and sleep apnoea differ
Measures that may help both conditions
Improving nasal airflow is often an important first step. Addressing congestion or structural nasal problems can reduce snoring and improve sleep comfort. Lifestyle adjustments, such as weight management and limiting alcohol before bedtime, are commonly advised.
First-line treatment for confirmed sleep apnoea
Positive airway pressure therapy remains a cornerstone treatment for many patients. It keeps the airway open during sleep and prevents repeated collapse. People searching for ent doctor for sleep apnea are often introduced to this option early in their care journey.
Oral appliances for selected patients
Custom-made oral appliances may be suitable for some individuals with milder disease. These devices work by gently repositioning the lower jaw forward during sleep. Regular review is essential to ensure effectiveness and comfort.
When procedures or surgery are considered
Procedural or surgical options are considered when specific anatomical factors play a significant role. These may involve the nose or throat and are carefully selected. Surgery aims to improve airflow or support other therapies rather than replace them entirely.
When should an ENT doctor be consulted?
Symptoms that warrant specialist review
Persistent loud snoring combined with breathing pauses or gasping should always be evaluated. Significant daytime sleepiness, poor concentration, or morning headaches are also warning signs. These symptoms suggest a higher likelihood of sleep apnoea.
Structural or nasal symptoms
Long-standing nasal blockage that interferes with sleep is a valid reason for ENT consultation. Difficulty breathing through the nose can worsen snoring and sleep-disordered breathing. Treating nasal issues can lead to meaningful improvement.
Children and special considerations
Children who snore frequently should not be overlooked. Enlarged tonsils or adenoids are common contributors in younger patients. Early assessment can prevent long-term sleep and behavioural problems.
When treatment decisions become complex
Patients who struggle with therapy tolerance or have persistent symptoms benefit from specialist input. An ENT doctor can help clarify the diagnosis and tailor management. This is particularly relevant for those exploring sleep apnea treatment in Singapore and seeking a structured approach.
Practical questions to ask during your ENT visit
Understanding your diagnosis
Ask whether your symptoms suggest simple snoring or obstructive sleep apnoea. Clarify whether a sleep study is recommended and what information it provides. A clear understanding supports better treatment decisions.
Identifying the main problem area
It is helpful to ask where airway narrowing is most significant. Knowing whether the nose, palate, or tongue base is involved guides management. This also sets realistic expectations for outcomes.
Discussing treatment pathways
Discuss all suitable treatment options and their pros and cons. Ask about long-term management and follow-up needs. Shared decision-making improves adherence and results.
Conclusion
Snoring should not automatically be dismissed as harmless. When it is loud, persistent, and associated with disturbed breathing or daytime impairment, further evaluation is justified. An ENT assessment helps determine whether sleep apnoea is present and ensures that treatment is appropriate.
Early recognition and timely intervention can improve sleep quality, daily functioning, and overall well-being. When in doubt, seeking professional advice is always safer than assuming symptoms are normal.